What are the signs of dental implant failure?
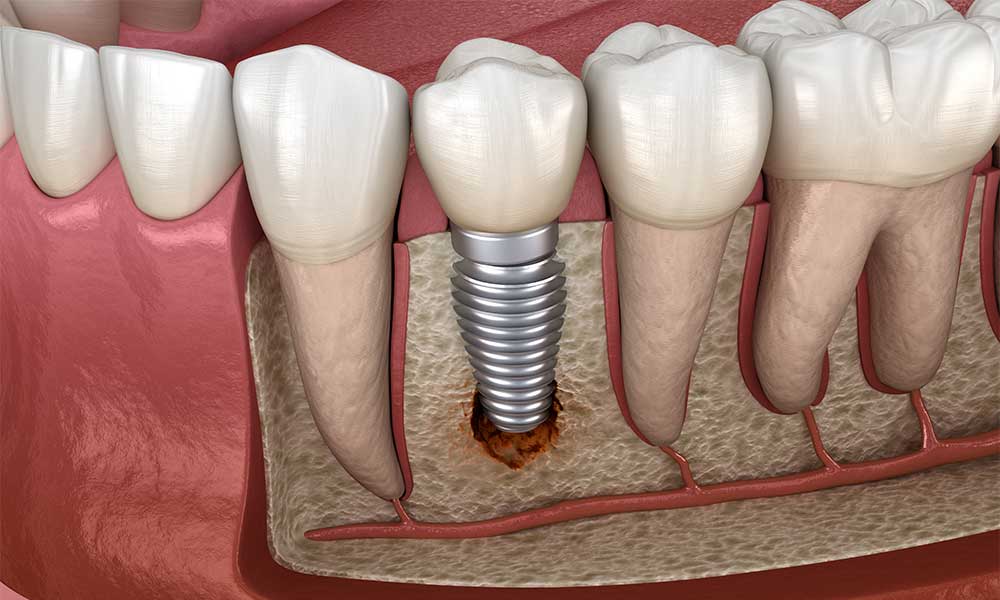
Table of Contents
What are the signs of dental implant failure?
Here are three common ones.
1- Pain or discomfort
Though pain is part of the healing process for dental implants, it shouldn’t persist long after the procedure. Having the feeling that something isn’t quite right is reason enough to get a second opinion from your dentist.
2- Swelling, inflammation, or bleeding
Red and swollen gums are often a sign of a gum infection. Since infections often accompany implant failure, it’s best to get your implants checked out the moment you experience these signs.
3- A loose feeling
Osseointegration is the process of the fixture fully fusing with your facial bone. Before you lost your tooth, its root was fully connected to your jaw bone. Just so, the fixture will become one with your body during this healing process where it becomes a strong anchor. If the implant doesn’t feel stable or if it’s wobbly like the loose teeth of your childhood, it’s time to call your dentist.
Clinically, failing dental implants are characterized by soft tissue inflammation, increased probing depths, increased mobility, and peri-implant radiolucency. Changes involve both the hard and soft tissues surrounding an implant. The implant may exhibit all the signs of peri-implant mucositis, as well as exudate, an increase of pocket depth, and bone loss. If left untreated, significant bone loss, infection, and mobility could result, leading to the failure of an initially integrated implant.
Removal of supra-gingival plaque with use of toothbrushes can significantly reduce the amount and composition of the subgingival microbiota. This reduction should translate to decreased risk of periodontal disease initiation or recurrence. Furthermore, the decreased prevalence of periodontal pathogens in supra-gingival plaque lowers potential reservoirs of these species. The absence of adequate keratinized mucosa in dental implants, especially in posterior implants, was associated with higher plaque accumulation and gingival inflammation, but not with a more annual bone loss, regardless of their surface configurations.
The implant type, with the presence or absence of keratinized tissue, may be a challenge for oral hygiene procedures for many patients. The clinician should stress the importance of adequately performing plaque control and select products and procedures well suited to the needs and ability of the patient. Patients rely on clinicians to suggest or recommend products for oral hygiene procedures. As with most patients, the “tell-show-do” method of home care instruction is important.
Documentation in the patient record regarding recommendations and instructions, as well as the patient’s compliance and effectiveness, will be important to evaluate long-term success for each patient. When choosing and recommending implements for oral hygiene, the clinician should take into consideration the location, length, and angulations of abutments, superstructure design, anatomical limitations, patient habits, motivation, and manual dexterity of each patient. Contributing factors that may influence product selection are plaque and calculus accumulation, as well as the general health of the patient (including diseases and medications).
To avoid patients becoming discouraged and poorly motivated, it is wise to keep oral hygiene instructions simple. Partially edentulous patients exhibit higher pathogenic bacterial counts than edentulous patients, which may cause seeding of pathogenic bacteria from one site to another. The final prosthesis should allow for access by the patient and clinician to keep the areas plaque free. The clinician should instruct the patient in the use of toothbrushes (manual or automatic); floss (with threading devices, if necessary); tufted brushes; inter-dental brushes (with coated wires); toothpicks; and oral irrigators. Patient instructions may include the use of readily available antimicrobial toothpaste products on grocery or pharmacy store shelves. They include many national brands. Dentists can make a recommendation on a product.
If oral irrigation is used, the patient should be instructed to use the lowest setting and direct the irrigation flow through the contacts to avoid excessive pressure to the implant tissue cuff. Incorrect use could alter tissue adaptation and induce bacteremia around the implant. Additionally, clinicians should recommend that the patient be gentle, yet thorough, post-surgically to avoid complications of healing from aggressive hygiene procedures.
The role of the dental hygienist in implant maintenance is growing. The hygienist can play a part in
- Identification of potential implant patients
- Education and motivation throughout treatment
- Development, continual assessment, and modification of patient-specific oral hygiene procedures
- Evaluation of prosthesis (components, attachments, mobility, and retention)
- Evaluation of peri-implant tissue
- Exposure of clinically acceptable radiographs
- Removal of biofilms, soft and hard accretions
- Recommendation of oral hygiene implements
- Determination of a patient-specific recall interval
- Identifying potential problems or complications
- Documentation of implant status
What are the causes of dental implant complications?
There are a few complications that cause dental implant failure. Here are the most common reasons why implants don’t function properly.
- Peri-implantitis
- If the fixture fails to integrate into your jaw
- Damage to nerves or tissue
- Sinus issues
- When too few implants support too many prostheses
- Allergies
- Gum disease
The differences between a tooth and implant biologies make dental implants more susceptible to inflammation and bone loss in the presence of bacterial plaque accumulation. Biofilms are the primary causative factor of periodontal disease processes. Sticky masses of bacteria with a polysaccharide matrix, water, and bacteria accumulate on hard and soft surfaces in the oral cavity and can be disturbed and removed with mechanical or chemical obliteration. If undisturbed, mature plaque will form.
Current medications cannot penetrate thick biofilm, and rough surfaces have been found to hold more biofilm than smooth surfaces. Bacteria will move from teeth to implants and from an implant to implant. Similar to teeth, clinical findings of failing implants include inflammation, pockets, and progressive bone loss.
When evaluating the peri-implant microbiota, a study compared microbial changes between patients with a history of periodontal or peri-implant infections and implants that have been in function for a length of time. This study found a history of periodontitis had a greater impact on the peri-implant microbiota than implant-loading time. The major influence on the peri-implant microbiota was, however, the microbiota on remaining teeth.
Thus, it is important to educate patients about their responsibility to decrease plaque effectively, especially if they have a history of periodontal disease. Plaque biofilm development and maturation have similarities for natural teeth and dental implants. The gingival sulcus in periodontal health and the peri-mucosal attachment of a successful dental implant are essentially similar.
What are the most common complications of implants?
The most common complications of dental implants are related to biomechanical lapses and conditions. Implant failures may result from the micromovement of the implant from too much stress placed upon it. Prostheses or abutment screws may become loose from bending or moment forces. The implant or component fracture may occur from fatigue conditions. Prosthesis failure may result from all of the foregoing or bending fracture resistance. Also, the manifestation of biomechanical loads on dental implants (moments, stress, and strain) controls the long-term health of the bone-implant interface.
- Fixture- This is the “base” that’s essentially a screw-shaped anchor inserted into your jaw bone and gums. It’s installed first and allowed considerable time to heal and fully integrate with your bone. When successfully implanted, fixtures are not much different from natural teeth roots.
- Abutment- This is the part that extends from the fixture. After the abutment is installed, any compatible dental prosthesis can be anchored to it. False teeth like bridges, crowns, and dentures can be attached to abutments, serving as comfortable and natural-feeling teeth replacements.
What is the failure rate of dental implants?
In a recent study by the American Association of Endodontists, the failure rate of dental implants is a minimal 1.6%. In their research, there were just two failures out of 129 dental implant procedures, showing how proper procedures can greatly increase the chance of dental implant success. Other sources report a failure rate of 5%— which is still an extremely low figure.
Implant success is as difficult to describe as the success criteria required for a tooth. A range from health to disease exists in both conditions. The primary criteria for assessing implant quality are pain and mobility. The presence of either greatly compromise the implant; removal usually is indicated. Probing depths may be related to the presence of local disease or preexisting tissue thickness before the implant was inserted. An increasing probing depth is more diagnostic and signifies bone loss, gingival hyperplasia, or hypertrophy. Bone loss usually is evaluated best with probing rather than with radiographs. The most common cause of bone loss during the first few years of function is related to factors of stress. The bleeding index is observed easily and indicates inflammation of the gingiva. However, implant health status is not as related to sulcular inflammation as would be the case with a natural tooth.
Implant failure is easier to describe and may consist of a variety of factors. Any pain, vertical mobility, uncontrolled progressive bone loss, and generalized peri-implant radiolucency warrant implant removal of the implant(s).
What is peri-implantitis?
Peri-implantitis is a complication that can happen with dental implants. It’s characterized by an infection and inflammation of the tissue surrounding the dental implant. This complication has two phases: infection and deep inflammation.
- The infection stage: This is when the gum tissue around your implants get infected with bacteria. Swelling, redness, and some bleeding is a sign of this stage, much like gingivitis. Thankfully, this situation can usually be reversed by good home care. If the inflammation is due to some excess dental cement leftover from attaching the prosthesis, then a visit to your dentist to remove the cement can resolve the issue.
- The deep inflammation/infection stage: This is when the situation has been left to its devices for too long, and the infection has reached the bone. When the bone gets compromised from the infection, the support for the implant wanes. This is the stage when there’s bone loss, and bleeding.
Can you have a dental implant removed?
Yes. Dental implants can be removed and inserted after the proper precautions have been made. Your dentist will need to clean the tissue around your failed implant and make sure the entire surface is free from harmful bacteria. You may need graft material placed that will regrow the bone around the failed implant. When the site is ready to receive a dental implant once more, there should be no issues in trying to insert a new fixture.
If you have any more questions about dental implants and their benefits and risks, contact us.
How long do dental implants last?
Your dental implants can last for a long time with proper care. The base of dental implants is made of non-corroding titanium that should become part of your body. In fact, implants can last for decades when they are maintained, cleaned, and checked up on regularly.
Do I need to brush dental implants?
Absolutely. Taking care of your implants just like they are regular teeth will maximize your chances of keeping them functional for as long as possible. Make it to every dental appointment, cleaning, and check up to make sure everything is how it should be.
Patients must be thoroughly educated and retrained before deciding to place implant. The ability of the patient to understand financial, time, and maintenance obligations is crucial.
In addition to educating patients, clinicians will need to assess compliance with a home care routine’ and must possess the clinical competencies to perform maintenance procedures. As the number of dental implants placed in patients continues to increase, there is a need to understand the importance of maintenance as it relates to long-term implant success. The role of the dental hygienist in implant maintenance and care is increasing and becoming more defined over time as more patients are seen by hygienists and protocols for the successful result of implants are drawn.
Implants and their prosthetic devices are different from natural teeth and may require different procedures and instruments for both professional and patient care. Instruments must be effective at removing biofilms and accretions, and procedures performed by patients and/or clinicians should avoid damage to all portions of the implant, abutment, restoration, and tissues. Establishment and maintenance of a soft tissue seal around the transmucosal portion of the implant can enhance the success of an implant. This barrier is fundamentally a result of wound healing. The maintenance of healthy peri-implant tissues may contribute to implant success factors issues and an implant sulcus free of inflammation and infection and with an absence of virulent bacteria can enhance a patient’s general and oral health.
Can you break a dental implant?
The short answer is yes. The good news is that it’ll be hard to do because dental implants are strong. You’re going to have to do the things that would break natural teeth. For example, you need to recklessly chomp on jawbreakers, participate in extreme sports, or completely neglect self-care and develop gum disease. If you are a teeth grinder or have bite issues, this can also lead to a dental implant fracturing or break off.
-
December 09, 2021Dental Implant Cost & Care
-
October 04, 2021Full Mouth Dental Implants Cost and Procedure
-
September 16, 2021Dental Bone Graft Cost, Materials and Procedure
-
June 15, 2021What is the average cost of Snap on?
-
May 27, 2021A Complete guide to Dental Implants Process and Timeline
-
May 10, 2021What Can You Do for Missing Teeth?
-
May 09, 2021What is The Cost of Single Tooth Implant?
-
January 17, 2021Do I Need Medical Clearance Before Dental Surgery?