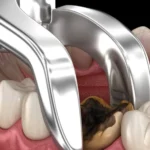
Do I Need Medical Clearance Before Dental Surgery?

What is the primary reason for medical clearance before dental surgeries?
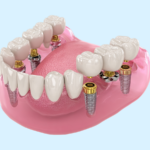
Understanding the medical history and obtaining medical clearance of each patient undergoing any kind of dental surgery is of primary concern of our oral surgeons. Each person receiving implants will be carefully evaluated to determine whether their health is appropriate for implants.
In that respect, written medical histories are taken for every implant surgery candidate. The patient’s medical history is taken the first time the surgeon speaks to the patient to learn about his/her health past and current conditions. Time and consideration are taken at the onset of optimizing the subsequent treatment and care process. The health history is recorded during the medical evaluation to give the practitioner a thorough understanding of the patients’ medical history and listed conditions and any common problems.
Two basic categories of information are addressed when the medical history is taken, including a review of the patient’s systemic health. The dentist uses a medical evaluation to obtain most of this information. Of particular note are medication usage within the preceding six months, allergies, and a review of the systems of the body. The pathophysiology of the systems, the degree of involvement, and the medications being used to treat various conditions are discussed.
Why do we refer a patient for a consultation?
On the basis of medical history, physical examination, and laboratory screening, contact with the patient’s physician for consultation or referral purposes may be warranted. A phone call for a quick consultation is useful but medical clearance has to be in writing from the patient’s physician through a mail or fax. The physician will assess the risk of dental surgery based on the patient past and current condition in four categories:
ASA I Normal healthy patient
ASA II Patient with mild systemic disease
ASA III Patient with moderate systemic disease
ASA IV Patient with severe systemic disease
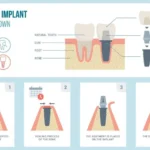
Why is medical clearance important before implant surgery?
The medical evaluation is really important before implant surgery, perhaps more so than in other disciplines of dentistry. Implant treatment is primarily a surgical, prosthetic, and maintenance discipline for an older segment of the population. The need for treatment increases with the age of the patient; as a result, the implant dentist treats more elderly patients than do other specialists in dentistry. An estimated 12 percent of the U.S. population is 65 years of age or older; this number is expected to reach 21 percent in the year 2030.
Physiologic changes associated with aging and their pharmacologic counterparts modify the physical, social, and economic life of the patient. Older adults (65 and older) have become an increasingly large segment within dental practices, especially in dental implant cases. The aging patient’s baseline health state can sometimes be complicated by conditions such as hypertension and diabetes) and other changes associated with aging. Older adults may use a number of prescriptions or other medications and special attention to adverse drug reactions must be taken in their dental care.
Although important individual variations exist, the biological systems of the elderly patient must cope with a decrease in function and physiologic reserve. These physiologic changes may predispose or increase the aging patient’s susceptibility to disorders. In general, a healthy older person demonstrates only half the lung function of a healthy young adult. The blood flow of an older patient is 80 percent that of a healthy 30-year-old patient, the cardiac output is only 70 percent, the renal plasma flow is only 50 percent, and the glomerular filtration is only 60 percent. A decrease in the elasticity of the arterial system is illustrated by an increase in systolic blood pressure. The vital capacity is reduced to 70 percent of a 17-year-old patient and corresponds to a decrease in the arterial partial pressure of oxygen.
Gastric motility and intestinal absorption are also decreased. The total bodyweight of the patient is often reduced, especially if masticatory deficiency from lack of teeth and bone is present; however, there is an increase in body fat. Consequently, any medications administered will follow modified pharmacokinetics and dynamics. Drug kinetics are modified, especially in the distribution phase, as a result of the increased water weight, decreased plasma albumin, and decreased cardiac output. The decreased plasma albumin concentration causes a greater percentage of the drug to remain free and active. The decreased ability to metabolize drugs, related to the decreased renal function, is responsible.
In addition to a medical history being taken, a medical physical examination should be undertaken. A complete evaluation of the head and neck is important initially and at all subsequent preventive maintenance (recall) appointments. The patient is informed of the need for periodic examination for cysts and benign or malignant tumors (26,000 cases of cancer are diagnosed in the head and neck region each year).
The extraoral examination is performed first. Features and facial symmetry are observed, including the ears, nose, and eyes. If the midline, occlusal plane, or smile line of the natural teeth or existing prosthesis is not harmonious, the cause should be determined. The submental, submandibular, parotid, and cervical areas are palpated for lymphadenopathy or unusual swelling. The area between the cricoid notch and the suprasternal notch is palpated for hypertrophy of the thyroid gland because its physiology influences bone metabolism and implant management.
Intraoral examination of the lips, labial and buccal mucosa, hard and soft palate, tongue, and oral pharynx is then performed. Any lesions or disease states must be further evaluated before implant procedures commence.