What Is Condensing Osteitis?

Condensing osteitis, also sometimes referred to as focal sclerosing osteomyelitis, is a dental condition that is technically considered to be a periapical inflammatory disease. Condensing osteitis is a dental condition that you might never have heard of before. While condensing osteitis is not a very common issue, it does sometimes occur even in patients who are responsible for making an effort to take good care of their teeth. When it is diagnosed by your dentist, they will most likely recommend that you make an appointment or give you a referral to see an endodontist for the next step of your treatment.
We have compiled some useful, general information about this condition below to answer some of the questions or concerns that you may have about the causes and possible treatment options for condensing osteitis.
Table of Contents
What is Condensing Osteitis?
All of your teeth are kept in place by the root or roots that extend from inside your tooth into your jawbone. Your front teeth typically have one root, but your other teeth have two or more. The tips of these roots are what is known as the apex. The apex is also where blood vessels and nerves enter your tooth and where they travel through the root canal into the pulp chamber. The pulp chamber is protected by the crown of your tooth, which is the part of your tooth that is visible in your mouth above your gums.
Condensing osteitis, also sometimes referred to as focal sclerosing osteomyelitis, is a dental condition that is technically considered to be a periapical inflammatory disease. The word ‘periapical’ refers to something that either relates to, occurs in, or affects the tissues that surround the apex of the root of your tooth.
Condensing osteitis, while considered an inflammatory disease, is more of a reaction to stimulus from inflammation. While this is most often a periodontal infection, this condition can be caused by other forms of inflammation as well. Condensing osteitis is a little unusual as far as a response to infection goes because it increases the production of bone rather than causes the destruction of it, which is the more common response to an inflammatory disease of this nature. This bone production will usually result in a radiopaque lesion.
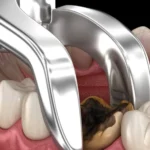
When something is radiopaque, this means that it prevents radiation from passing through it. A good example of something radiopaque that you might be familiar with is the way metal looks in an X-ray. If you’ve ever seen an X-ray of, for instance, someone who has a metal plate in their body, the metal stands out as a solid object against the rest of the X-ray. This is similar to the way a radiopaque lesion appears in an X-ray of your teeth.
Because this condition is usually asymptomatic, and only occasionally causes tenderness and pain, the presence of one of these dense, radiopaque lesions on an X-ray is most often the way that your dentist or endodontist will identify and diagnose you. Condensing osteitis is most commonly a condition that develops in young adults, but it can also occur at any age. Most cases are found in the premolar/molar region of the mouth.
What causes Condensing Osteitis?
When you have a dental infection in the periapical region of a tooth, this inflammation can sometimes cause a sclerotic reaction in your tooth, which increases your bone density in the area. This increase in bone density is what will make the tooth appear radiopaque in a dental X-ray. Patients who develop condensing osteitis are almost always individuals who have a very healthy immune system. The robust response of their immune system to the infection combined with bacteria that has a low degree of virulence from the infection is what triggers the sclerotic reaction that causes condensing osteitis.
How is Condensing Osteitis treated?
When your dentist believes that they have determined that you have condensing osteitis, the best course of action is to refer you to an endodontist. At your endodontic appointment, your tooth will need to be examined. The endodontist will take a good look at the area around your tooth and will also need to test the vitality of the pulp within it.
This is done by a vital pulp test (VPT). Endodontists test pulp with a combination of four possible methods:
● Cold test
● Hot test
● Electric test
● Cavity test
The combination of testing that your endodontist chooses will be determined based on your primary complaint. For example, if you don’t have any existing thermal pain or sensitivity in the area, a cold or hot test will be employed. The electric test requires specific conditions to perform and is not always practical. The cavity test is considered a last resort, as it involves stimulation of the pulp without the use of anesthetic. Vital pulp will have a pain response to this stimulation.
If the pulp in the sclerotic tooth has become necrotic or has developed an irreversible level of pulpitis, which is a severe inflammation of the dental pulp, then the tooth may be impossible to restore properly and will need to be extracted.
What is the prognosis for Condensing Osteitis?
It may be surprising to hear, but if the sclerotic tooth is not infected, is free of uncomfortable or painful symptoms and is benign, there isn’t any necessary treatment for the tooth. It can remain where it is and function regularly, sometimes for many years without change. It will be necessary for you to have periodic radiographs of the tooth to monitor any changes that might occur over time and correct them if needed.
If the tooth does require extraction, you might be left with an area of condensing osteitis in your jaw. This is known as a bone scar, or osteosclerosis and is not painful.
-
February 15, 2023What Is The Average Cost Of Braces In Houston?
-
February 01, 2023What You Need to Know About Dental Hygienists?
-
January 30, 2023What to Expect During the Wisdom Teeth Extraction
-
October 23, 2022Wisdom Tooth Removal Cost
-
October 23, 2022Dental Emergency, Open Saturday
-
October 23, 2022Full Guide to Dental Crown
-
July 26, 2022Should I Have My Wisdom Teeth Removed Before I Get Braces?
-
July 26, 2022Complete Guide to Wisdom Tooth Removal