What You Need To Know About Tooth Extraction
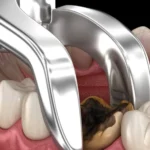
In today’s modern world of dentistry, tooth removal can take on many different forms. Fortunately, patients have more choices today than ever before when it comes to extracting teeth as well as replacing those teeth. In many instances, tooth removal refers to the extraction of wisdom teeth. However, there are many cases where tooth removal involves some other teeth for various reasons. From facial trauma to tooth decay and a wide range of different situations, teeth may be so severely damaged that they just cannot be saved and, as such, must be removed. Fortunately, tooth extraction is a safe and reliable type of dental procedure that is performed thousands of times a day across the country.
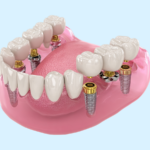
A general dentist is often able to extract teeth with outstanding results. However, there are instances where tooth extraction is considered to be more complex, thus requiring the assistance of an oral surgeon. Patients should understand that subsequent removal, some tooth replacement option is recommended. This helps to restore the patient’s smile, overall appearance, and oral functionality. Tooth replacement can involve a permanent fix bridge as well as complete upper or lower dentures or dental implants.
Table of Contents
Why Sometimes Wisdom Tooth Needs To Be Removed?
- Extraction is considered a good option when one or more wisdom teeth have grown in or erupted at an unusual or awkward angle. In other words, the tooth may be facing backward, forward, or tilted to either side.
- In other instances, extraction is recommended when the patient’s jaw is not large enough to support this kind of tooth once it has grown in fully. When the jaw is not sufficient enough in size to support a wisdom tooth, the tooth may become impacted. An impacted tooth is simply a tooth that is unable to break through the gums as it normally would otherwise.
- Wisdom tooth extraction is often recommended when the tooth breaks only part of the way through the gums. This results in a flap of gum tissue that grows over the tooth. The result can be infections caused by germs that become trapped within the skin flap. In this situation, gums can become painful, swollen, and red in response to chronic disease.
- Tooth removal is usually the best choice when dealing with impacted teeth. This is generally because of more severe problems such as infections, cysts, or damage to bone and teeth can ultimately occur when an impacted wisdom tooth is left untreated.
The extraction of a wisdom tooth is usually accomplished by a dentist or an oral/maxillofacial surgeon in an outpatient environment. Depending on the severity of the patient’s condition, the surgery may, in some instances, require hospitalization. Patient hospitalization is more common when all wisdom teeth must be pulled in one procedure, especially for those who are considered high risk for complications. As a note, patients with an infection may be required to take antibiotics for the infection to subside before surgery can be performed.
Wisdom teeth removal can involve the use of local or general anesthesia, depending on each case. General anesthesia is more commonly used when all wisdom teeth are to be removed at the same time. Wisdom tooth extraction involves the dentist opening up the gum tissue over the tooth and removing any bone covering the tooth. Once tissue connecting the tooth to bone has been separated, the tooth can be safely removed. In some cases, stitches may be required. Fortunately, today’s modern stitches will dissolve over time, while other older types of stitches may need to be removed a few days later.
Wisdom tooth extraction typically is an outpatient procedure. Perhaps most encouraging of all is that it only takes a few short days to heal and recover from the procedure thoroughly. In fact, patients are usually returned to their routine faster than might be expected. The real question becomes why take wisdom teeth out in the first place?
In the most basic of terms, wisdom teeth are third molars. This particular set of teeth typically comes in somewhere between the ages of 17 and 25. That said many people go through an entire lifetime with perfectly healthy molars that never require treatment or extraction. Conversely, there are others who will at some point need wisdom tooth extraction to maintain optimum dental health. Here are a few examples of when this would be the case.
- If the patient’s mouth is not large enough to accommodate the introduction of molars they must be removed. In essence, the jaw has no available room for an additional set of teeth as they emerge.
- When a patient has an impacted wisdom tooth, extraction is normally recommended. This is especially true because wisdom teeth are located so far back within the oral cavity. An impacted tooth can be trapped in the jawbone or even inside the gums. The result is a painful and uncomfortable experience.
- If a patient has molars with cavities or gum disease, it may be due to regular oral hygiene such as flossing and brushing is not possible because the wisdom teeth were simply not accessible.
- There are other cases where wisdom teeth may erupt at an angle and press against the patient’s other surrounding teeth. This is another instance where extraction is usually recommended.
Impacted Wisdom Teeth
Commonly known as wisdom teeth, the third molars are the last teeth to erupt at the very back of the mouth behind the second molars. In most cases the final development of these teeth occurs during the middle teenage years and as late as the early 20s. These teeth are called wisdom teeth because they signify a time that is traditionally known as the onset of maturity where wisdom is ultimately gained. One issue that sometimes arises about wisdom teeth development is when they develop or erupt in an impacted way. This is sometimes experienced when the jaw is too small to accommodate the future developmental growth of wisdom teeth. When inadequate space is the issue, wisdom teeth that erupt irregularly are considered impacted.
Impacted wisdom teeth can affect regular oral hygiene, chewing and other types of typical dental functionality. Generally speaking, there are three types of impactions that should be considered. This includes soft tissue impaction when there is simply not enough room to allow for the retraction of gum tissue. This can have an effect on the patient’s ability to clean and care for teeth appropriately. Conversely, a partial bony impaction results when there is enough space for the tooth to partially but not completely erupt. In this case, the tooth is often unable to function in the right way about chewing and oral hygiene. Finally, there is the complete bony impaction type of wisdom tooth irregularity. This results when there is simply no room for the tooth to erupt naturally. The tooth remains completely embedded within the jawbone ultimately requiring some degree of surgical procedure for removal. Most notably, this type of impaction may include the tooth being in an unusual position making it very difficult to remove.
How is a Wisdom Tooth Removed?
Routine wisdom tooth removal begins with an examination and an x-ray of the patient’s mouth. This allows for the dentist to evaluate the position of the wisdom teeth and if any action is required. In most cases, early treatment offers better results for patients. Most dental care providers recommend initial evaluation of the patient for wisdom tooth development during the mid-teenage years. An orthodontist, maxillofacial surgeon or general dental care provider can do the assessment as required. Ideally, wisdom teeth that are impacted should be removed earlier rather than later. This is usually recommended because the root structure is not fully developed making removal easier. Those who wait until later in life to have wisdom teeth removed may experience complexities and problems that would not have been the case had the teeth been removed at an earlier age.
What to Expect After Tooth Extraction?
In most situations, wisdom tooth extraction is performed under local anesthesia or nitrous oxide (laughing gas). Once the procedure has been completed, the gum is sutured, and a gauze pad is placed in the patient’s mouth as a way to help control bleeding. Initially, the patient will rest under dental care or supervision in the dentist’s office until it is time to be taken home by a family member or friend. The patient is sent home with a post-operative instruction kit and a pain medication prescription. Most frequently a follow-up appointment is scheduled for about one week after the initial surgery to allow for routine suture removal.
What to Expect Post Wisdom Tooth Surgery
The good news for those who require wisdom tooth removal is that the entire procedure can be done in an outpatient environment where recovery only requires a few short days. Painkillers are, in many cases, prescribed by the doctor. That said, here are some excellent tips on how to speed up the recovery process after having wisdom tooth extraction surgery.
- While your mouth is still numb, it is best to avoid biting your lip, cheek, or tongue.
- Your dentist may also suggest that you not lie flat as this could promote excessive bleeding. Choose instead prop your head up with pillows to ensure less bleeding and a faster recovery. It is also recommended to avoid strenuous physical activity, as this may also cause excessive bleeding.
- Patients are instructed to gently bite on gauze padding occasionally as a way to promote healing. Patients with excessive bleeding that continues for more than 24 hours after surgery should contact their dentist or oral surgeon as soon as possible.
- It is recommended to continue usually brushing, but gently the following surgery. Patients are advised to avoid using a straw for drinking liquids for the first few days following surgery. Sucking through a straw causes negative pressure in the mouth and could result in the formation of a blood clot.
- Rinsing the mouth with warm salt water for the first few days following surgery is another excellent way to promote faster healing. This can be done several times a day to relieve pain and reduce swelling. In most cases, one tablespoon of salt in eight ounces of warm water will suffice. Always rinse gently so that the surgical site is not disturbed.
Oral Surgery Consultation
A typical scenario includes the patient first meeting with an oral surgeon to discuss the extraction process. Patients should expect to talk about their general health as well as any dental health related problems with their dentist. Also, patients should let their doctor know about any drugs they are currently taking and discuss the type of anesthesia that will be used. Most people typically choose between various general anesthesia and local anesthesia methods. Besides, timelines will be explained about how long recovery will be expected take. This allows patients to plan accordingly about school or work.
During The Tooth Removal
During the actual surgery, the first step usually involves the administering of anesthesia. If local anesthesia will be used, the dentist will numb your mouth with a routine shot of Novocain that takes effect quickly. Other options include a nitrous oxide or what is known as laughing gas. This allows the patient to relax and even take a nap during surgery. Still, other options include IV sedatives intended to make the patient drowsy and less aware of the procedure as it is taking place. Finally, general anesthesia is administered intravenously or can be administered via breathing gas. In this situation, the patient is soundly asleep throughout the duration of the procedure.
As the actual procedure progresses, the doctor will cut into the gums and bone as a way to safely extract the wisdom teeth. Eventually, the wound will be stitched closed to facilitate quick healing. Stitches are often of the dissolving variety precluding the requirement for the patient to return to have stitches removed. Patients can also expect to have gauze pads placed in their mouth to absorb any residual blood.
What To Expect Following Surgery
While each patient responds in varying ways to anesthesia, those who have had local anesthesia will typically be alert and able to drive a vehicle immediately following treatment. In some cases, patients are even permitted to return to work and resume normal activities on the same day following surgery. Those who have had general anesthesia may experience drowsiness and in most cases should not operate a motor vehicle.
Fortunately, most patients feel little to no pain following surgery. A small amount of swelling and minor discomfort may be experienced for a few days following surgery. Ultimately, the patient’s mouth will require a few weeks to heal completely. For the first three days following surgery here are a few tips worth considering.
- Plan to call your doctor immediately if pain or swelling does not dissipate or fever develops.
- Plan to use an ice pack on the affected side of the face as a way to reduce swelling.
- Take the medications as prescribed by your doctor to ease swelling and pain.
- Do gentle jaw exercises by opening and closing your mouth multiple times.
- When brushing teeth avoid making contact with blood clots. As a note, patients should wait to begin brushing their teeth until the second day following surgery.
- Drink adequate amounts of fluid and eat soft foods such as rice, pasta or soup.
There are many things that patients should also avoid if at all possible. This includes not smoking as it can slow healing. Refraining from eating crunchy foods, hard candy or any sticky foods that could interfere with the normal healing process is advised. Besides, patients should avoid rinsing their mouth too vigorously as this can also slow the healing process. Finally, avoid drinking with a straw as this may cause blood clots to loosen and thereby prevent normal healing.
Patients should know that wisdom tooth extraction is a routine procedure that is done countless times each and every day across the country. Consult with your dental care provider regarding your individual case to learn more.
Impacted Canines
While most cases involving impacted teeth focus on the wisdom teeth, there are situations where the canine teeth can become impacted as well. Any tooth impaction is a concern because of the potential for infections, chronic pain, and functionality problems. In the case of wisdom teeth, simple extraction is usually the best option because there is a minimal functional need for this particular type of tooth. About the maxillary canine, also known as the upper incisor tooth or cuspid, the tooth plays a critical role in maintaining a normal dental arch and a healthy bite. In most cases, something known as aided eruption is used as a way to retain the tooth and provide the patient with normal healthy oral functionality.
Oral Pathology
The inner surface of the mouth is normally a healthy pink in color and appearance. When the skin within the mouth shows changes in color or general condition, this could be a sign of some oral pathological process taking place. Anything from sores that fail to heal or that bleed excessively to reddish patches or white patches on the inside of the mouth can indicate some level of oral pathology. Even a chronic sore throat, difficulty chewing, hoarseness or thickening lumps within the skin lining of the inside of the mouth may indicate that some level of pathology is occurring. Gum tissue, the roof of the mouth, the cheeks as well as the lips may all indicate oral pathology. The most concerning of all oral pathologies is oral cancer. That said, there are many other medical conditions that can result in warning signs associated with the oral pathological process.
What Is The Benefit of 3D X-Ray In Dentistry?
Today’s modern state-of-the-art dental systems, tools and technology have greatly benefited both the patient and the doctor. Now doctors can better diagnose potential issues associated with dental health in a more accurate and timely way. In contrast to a traditional CT scanner, a 3D imaging system offers more precise and crystal-clear digital imaging while at the same time giving the patient an absolute minimum in radiation exposure. This type of 3D system allows the doctor to perform a full variety of diagnosis and treatments in an outpatient office setting. This helps to reduce the number of visits required by the patient. Most importantly, the latest 3D technology made available to dental care providers allowed for more targeted scanning and improved overall evaluation. This results in better and more effective dental care.
Dental Anesthesia and Dental Sedation
Fortunately for dental patients today there are more options than ever before when it comes to anesthesia. In most cases the nature of the surgical procedure required dictates the type of anesthesia that will be most appropriate. Equally important when considering anesthesia is the general level of apprehension of the patient. Local anesthesia is often used for simple oral surgical procedures and routine tooth extractions. With the case of local anesthesia, the patient is fully aware and awake. Only a localized area is numbed thereby allowing the procedure to progress normally. Another option that patients have is something known as intravenous sedation. This type of sedation is used to calm the patient and is sometimes referred to as twilight sedation because the patient is not completely unconscious. Other options include nitrous oxide or laughing gas and general anesthesia. Nitrous oxide is typically preferred because the patient recovers quickly and can even drive home following the procedure.
Surgical Instructions
Patients preparing for oral or facial surgery normally receive surgical instructions from the dentist or oral surgeon. These types of instructions are provided about preparing for anesthesia as well as what to do after wisdom tooth removal or after dental implant surgery, for example. Detailed instructions on what to do following surgery are also provided to patients who have had multiple extractions or following the exposure of an impacted tooth. The patient working in unison with their dental care provider or oral surgeon is typically the best way to determine the best course of action about anesthesia for various dental procedures.
Before Anesthesia
The surgical instructions preceding anesthesia include having the patient avoid eating or drinking for at least six hours before their dental procedure. Instructions also include refraining from smoking for at least 12 hours before surgery. Patients are advised to have a responsible adult on hand following surgery. This ensures that the patient will get home safe and without incident. Patients are advised not to drive following a surgical procedure that involves anesthesia and should wear loose fitting clothes that are comfortable. Further, patients should not wear makeup, dentures, jewelry or even contact lenses.
After Wisdom Tooth Removal
Following wisdom tooth removal, patients are given instructions on what to do immediately after the surgery as well as for the second and third day. Initially, the patient is provided with gauze packs that are placed over the surgical site as a way to absorb any excess blood. Other general instructions include exercising care to ensure that the surgical area is not disturbed. Instructions are given on oral hygiene, acceptable activities as well as how to deal with any persistent bleeding, swelling or unanticipated pain. Instructions about how to brush and what to expect regarding normal healing are also standard following wisdom tooth removal surgery. Ultimately, talk with your dental care provider for a full and detailed list of exact surgical instructions following any oral surgery.
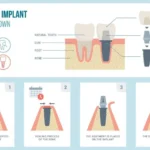
After Dental Implant Surgery
About dental implant surgery, the surgical instructions are similar to other types of oral surgery. Instructions will typically cover what to do within the first hour as well as how to exercise care and perform normal oral hygiene. Instructions will also talk about acceptable activities, what to expect about swelling, persistent bleeding or continued pain. Also covered in general instructions include what to do about nausea and the best type of diet to maintain immediately following surgery.
After Multiple Extractions
As with wisdom tooth removal surgery and dental implant surgery multiple-extractions related surgical procedures require specific surgical instructions to be followed by the patient. As mentioned above, there are certain instructions that must be adhered to during the first hour following surgery as well as maintaining proper care by conducting oral hygiene in a safe way that will not disturb the surgical site. Persistent bleeding, swelling, pain and other issues encountered following multiple extraction surgeries are also discussed in the surgical instructions provided by the dental care provider or oral surgeon.
After Exposure of an Impacted Tooth
The exposure of an impacted tooth through routine oral surgery also requires that the patient adheres to specific surgical instructions following the procedure. As with other types of oral surgery, surgical exposure of an impacted tooth requires that the patient exercise care and caution about not disturbing the site of the surgery. Instructions also cover oral hygiene, acceptable activities as well as what to do about swelling, pain or persistent bleeding.
Tooth Removal Cost
It is important to note that the pricing can vary substantially based on some factors. That said in most instances when a permanent natural tooth requires a simple extraction; the cost can range from around $150-$550. Conversely, when a permanent tooth requires surgical procedures for successful extraction, the cost can range from around $170 to about $620. Finally, a simple baby tooth extraction can cost around $85 to $160. Talk with your dental care provider for more specific pricing.
Successful Wisdom Tooth Extraction Surgeries
Consulting with your dental care provider is the best way to know for sure if wisdom tooth removal is right for you. Because each patient and each case are different, it is best to carefully consider your options when it comes to having this type of surgery performed. Tens of thousands of successful wisdom tooth extraction surgeries are performed every year, helping patients enjoy a better quality of life. Improved oral functionality and reduced incidences of dental disease are always the goals. Your oral surgeon can discuss the benefits and risks involved with having this highly successful dental surgery performed.
Final Thoughts
Whether wisdom teeth are removed because of impacted teeth that result in infection or removed as a preventative strategy, one thing is sure, and that is that today’s modern and advanced dental procedures, techniques and tools make this type of dental surgery safe and highly successful with patients of virtually any age. Staying proactive when it comes to dental health and oral hygiene is always the best approach.