Recent Posts
Dental Bone Graft Cost, Materials and Procedure
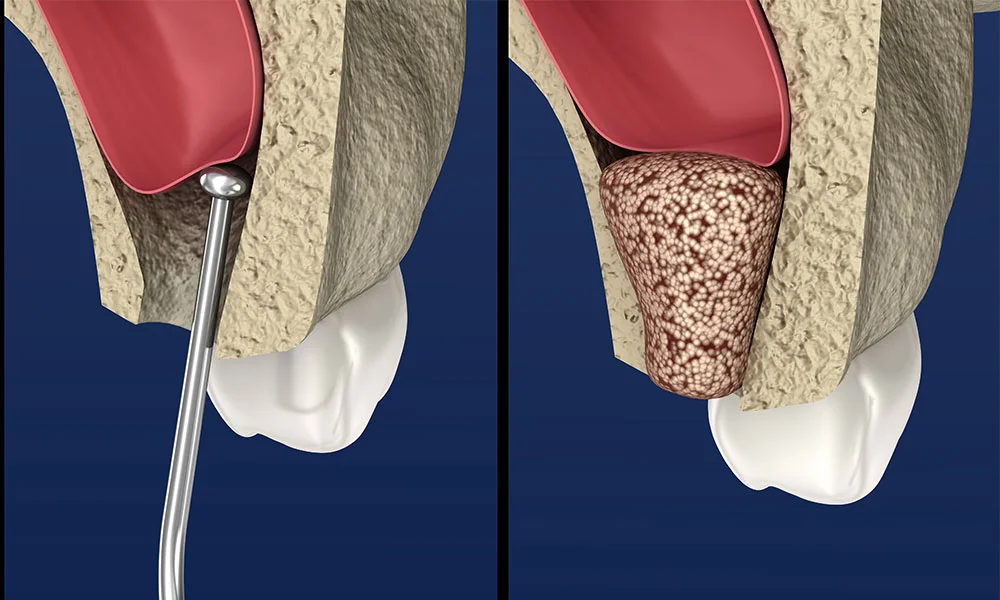
Table of Contents
Bone Graft Cost
If you’re researching bone grafts, chances are the cost is one of your biggest concerns — so let’s get into it.
For a basic graft using synthetic material on a single implant site, you’re typically looking at somewhere between $300 and $800. That’s the simpler end of things. Where it gets pricier is when the bone needs to come from your own body — say, your hip or chin. That kind of procedure means a hospital visit, plus you’ll need an orthopedic surgeon and an anesthesiologist in the room. All of that pushes the total up to roughly $2,500 to $3,500.
These are ballpark numbers, though. Every case is different, and there are a handful of things that can shift the price in either direction.
On top of the graft itself, there are usually some added costs to plan for. Your dentist will likely want a full set of x-rays, and in some cases a CT scan, before anything else happens. Those imaging procedures alone can add anywhere from $250 to $1,000 to your final bill.
One more thing worth doing early on: check with your insurance provider. Some plans cover bone grafting, some cover implants, some cover both, and some cover neither. It really depends on your policy, so it’s worth a phone call before you start making decisions.
What Is a Dental Bone Graft?
Not everyone has enough jawbone to support a dental implant — and that’s more common than most people realize. Your jaw needs a certain amount of bone density, height, and width for an implant to hold properly. This comes up a lot when someone has had a tooth pulled and wants to replace it with an implant down the road.
A bone graft is basically a way to build that foundation back up. Your dentist takes a close look at the jawbone — measuring its dimensions, checking the density — and figures out whether there’s enough structure to work with. If there isn’t, grafting fills in what’s missing so the implant has something solid to grab onto.
The good news is that grafting techniques have come a long way. Success rates are high, and for a lot of patients, it’s what makes the difference between being told “sorry, implants aren’t an option” and actually getting their smile back.
What Bone Is Used for a Dental Bone Graft?
There are four main types of grafting material, and each one has its pros and cons.
Autograft Bone
This is bone taken directly from your own body — usually the hip, chin, jaw, or sometimes near the knee. It’s widely considered the most effective option because your body recognizes it as its own, so the risk of rejection is almost nonexistent. The bone gets shaped to fit the area of your jaw that needs it.
The trade-off? You’re dealing with two surgical sites instead of one. The bone has to be harvested first, then placed. That means a longer procedure, more recovery, and a higher price tag.
Allograft Bone
This is donor bone sourced from a human cadaver, provided through regulated tissue banks around the country. Before it reaches you, the bone is freeze-dried and sterilized. It’s been used in dental work for a long time and has a strong track record. For patients who want to avoid a second surgical site, it’s a popular and more budget-friendly choice.
Xenograft Bone
This one surprises some people — it’s bone sourced from animals, most commonly cows. Despite how that might sound, it’s actually the most widely used grafting material in implant dentistry. Cow bone integrates with human bone remarkably well and rarely causes complications. It goes through the same freeze-drying and sterilization process as human donor bone, and it’s thoroughly cleaned before it ever gets near a patient.
Alloplastic Grafts
These are entirely synthetic — a lab-made mineral substitute designed to mimic bone. It fuses with your natural bone reliably, and it’s a solid option when biological materials aren’t the right fit for a particular patient.
In terms of effectiveness, the general ranking goes: your own bone first, then human donor bone, then animal bone, and synthetic material last. But “best” really depends on your situation — your health, the complexity of the graft, your budget, and what your dentist recommends. Have an honest conversation with them about which route makes the most sense for you.
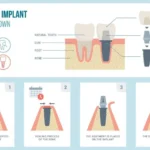
Dental Bone Grafting Procedure
Before the actual graft happens, there’s some prep work. Your dentist will start with x-rays to get a clear look at what’s going on under the surface. In more complex cases, they might order a CT scan, which gives them a detailed 3D image of your jaw.
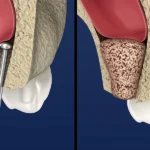
From there, they’ll figure out which type of graft you need. The main options are a socket graft (also called alveolar ridge preservation), a sinus lift, or a block bone graft. Sometimes patients need more than one type — it just depends on where the bone loss is and how extensive it is.
Once everything is planned out and the grafting material has been selected, the procedure itself is relatively straightforward. Your dentist places the material into the area that needs it, and then healing begins. Here’s the part that’s actually kind of fascinating: over time, your body gradually absorbs the grafted material and replaces it with your own natural bone. The graft is essentially scaffolding — it holds the space and gives your body a framework to rebuild around.
Frequently Asked Questions About Bone Grafting
1. How Long Does It Take to Recover From a Dental Bone Graft?
The first few days feel a lot like recovering from a tooth extraction — some tenderness, maybe a bit of swelling, nothing too dramatic. Most people are back to their routine within two or three days.
Full healing is a different story, though. You’ll need to wait about four to six months before the graft is ready to support an implant. That timeline depends on the individual — how well you heal, how closely you follow your post-op care instructions, whether you avoid messing with the surgical site. Cutting corners on aftercare is the quickest path to an infection, which can set the whole process back.
2. What Are Some Signs of a Failed Dental Bone Graft?
Infection is usually the first red flag. If you’re noticing pain or swelling that seems to be getting worse instead of better, get in touch with your dentist right away. They’ll take an x-ray to see if the graft has been compromised and whether it can still support an implant.
Certain things put you at higher risk for graft failure — smoking being a big one, along with diabetes. If either of those applies to you, make sure your dentist knows so they can plan accordingly.
3. Can a Bone Graft and Implant Be Done at the Same Time?
Sometimes, yes — if the amount of grafting needed is pretty minor. In those cases, your dentist can place the graft and the implant in a single visit. But if the grafting is more involved, the bone needs time to grow and strengthen before it can handle an implant. That usually means waiting several months between the two procedures.
4. Do Bone Grafts Hurt?
Most patients say they didn’t feel a thing during the procedure itself — you’re sedated, so it’s really not something you need to dread. If there’s any pain afterward, it’s usually tied to an infection during recovery rather than the graft itself. Stick to your aftercare routine and you should be in good shape.
5. Is It Necessary to Have Dental Bone Grafts?
It depends on how much bone you have to work with. If your jaw doesn’t have enough structure to hold an implant securely, a graft is really the only way to make it work.
Bone loss happens for all sorts of reasons — gum disease, grinding or clenching your teeth over the years, or simply losing a tooth and leaving the gap unfilled. Once a tooth is gone, the bone around it starts to shrink pretty quickly. And unlike some tissues in the body, jawbone doesn’t grow back on its own. So for a lot of people, grafting is what makes the difference between being a candidate for implants and not.
6. Is It Safe to Have Bone Grafts?
Yes — for the overwhelming majority of patients, bone grafting is very safe. If the material comes from a tissue bank, it goes through extensive screening. Donors are vetted thoroughly, all blood is removed from the tissue, and everything is tested for sterility and communicable diseases before it’s ever used.
If you’d rather use your own bone, that’s an option too, especially if you’re in good overall health. Just know that harvesting the bone adds a couple of extra days in the hospital for surgery and recovery.
There’s also something called an autograft, where your dentist uses bone from teeth that are already being extracted and grinds it down with specialized equipment. If you’re having any teeth pulled, it’s definitely worth asking your dentist whether this approach could work for your situation.
7. Do Most Dental Insurance Plans Cover Bone Grafting?
Here’s where things get a little tricky. Most dental insurance plans don’t cover implants, but some will cover part of the bone graft — especially if it’s been classified as medically necessary.
In cases where the bone loss was caused by an accident or a non-dental medical condition, your general health insurance might actually pick up some of the tab. And if bone loss has gotten severe enough that it’s affecting your ability to eat, there’s a chance both your dental and medical policies could contribute.
Your best bet is to review your policy or call your insurance company directly. And if cost is still a concern, ask us about financing — there are options out there.
8. Is Bone Grafting Necessary After Tooth Extraction?
In most cases, your dentist will do a socket preservation graft at the same time as the extraction. The reasoning is simple: bone loss starts immediately after a tooth comes out. Placing a graft right away helps keep the area intact so that when you’re ready for an implant later, the bone is still in good enough shape to support it. Skipping this step can mean needing a bigger, more involved graft down the line.
9. Can You Get Dental Implants With Bone Loss?
You can — as long as you’re a good candidate for bone grafting. Dental technology has advanced to the point where even significant bone loss doesn’t automatically rule you out. If you’re in decent overall health, a grafting procedure can rebuild what’s been lost and get you to a place where implants are viable.
Without grafting, though, severe bone loss pretty much takes implants off the table.
10. Are You Put Under General Anesthesia for a Dental Bone Graft?
It depends on how complex the procedure is. For smaller, more routine grafts, local anesthesia is usually enough — you’re awake but the area is completely numb. For bigger procedures, your oral surgeon might recommend general anesthesia so you’re fully asleep throughout. They’ll walk you through what to expect ahead of time.
11. How Do Bone Grafts Work?
At the most basic level, a bone graft provides the raw material your jaw needs to support an implant. Implants themselves are made from titanium alloy — a metal that bonds exceptionally well with human bone, which is why it’s the go-to material.
There are several grafting approaches depending on where the bone loss is: socket preservation grafts, lateral ridge preservation grafts, block bone grafts, and sinus lifts (which are specifically for the upper jaw). Your dentist will evaluate your situation and recommend the procedure that fits best.
See Also: Learn more about bone graft in dentistry at NCBI
December 09, 2021Dental Implant Cost & Care
October 04, 2021Full Mouth Dental Implants Cost and Procedure
September 16, 2021
Dental Bone Graft Cost, Materials and Procedure
June 15, 2021What is the average cost of Snap on?
May 27, 2021A Complete guide to Dental Implants Process and Timeline
May 10, 2021What Can You Do for Missing Teeth?
May 09, 2021What is The Cost of Single Tooth Implant?
January 17, 2021Do I Need Medical Clearance Before Dental Surgery?